SurgiClose is intact fish skin intended for the management of trauma wounds and surgical wounds in the operating room. Because there is no known risk of viral or prion disease transfer from North-Atlantic cod to humans, the fish skin only needs mild processing with our proprietary method.[2]
This process preserves the skin’s natural qualities,[2] including: its three-dimensional structure, mechanical properties, molecular organization, and composition.[1-4]
The product is homologous to human skin1 and when applied to damaged tissue, such as partial thickness burns or wounds, helps to support the body’s own cells to regenerate tissue.[5-12]
SurgiClose® Benefits
Promotes incorporation and cell ingrowth [1]
Preserved microstructure facilitates dermal regeneration [1]
Rapid neovascularization through naturally porous skin structure [1]
Natural barrier protecting against environmental threats [1]

Standard
SurgiClose is intact fish skin that comes in various sizes and variations.

Silicone
SurgiClose Silicone provides a breakthrough balance of protection, breathability, and stability with a combination of fenestrated fish skin and a highly-refined, porous silicone contact layer.
Now available in four new sizes that will accommodate smaller wounds ranging from a 3×3 cm bordered product to a 10×10 cm borderless version.
Micro
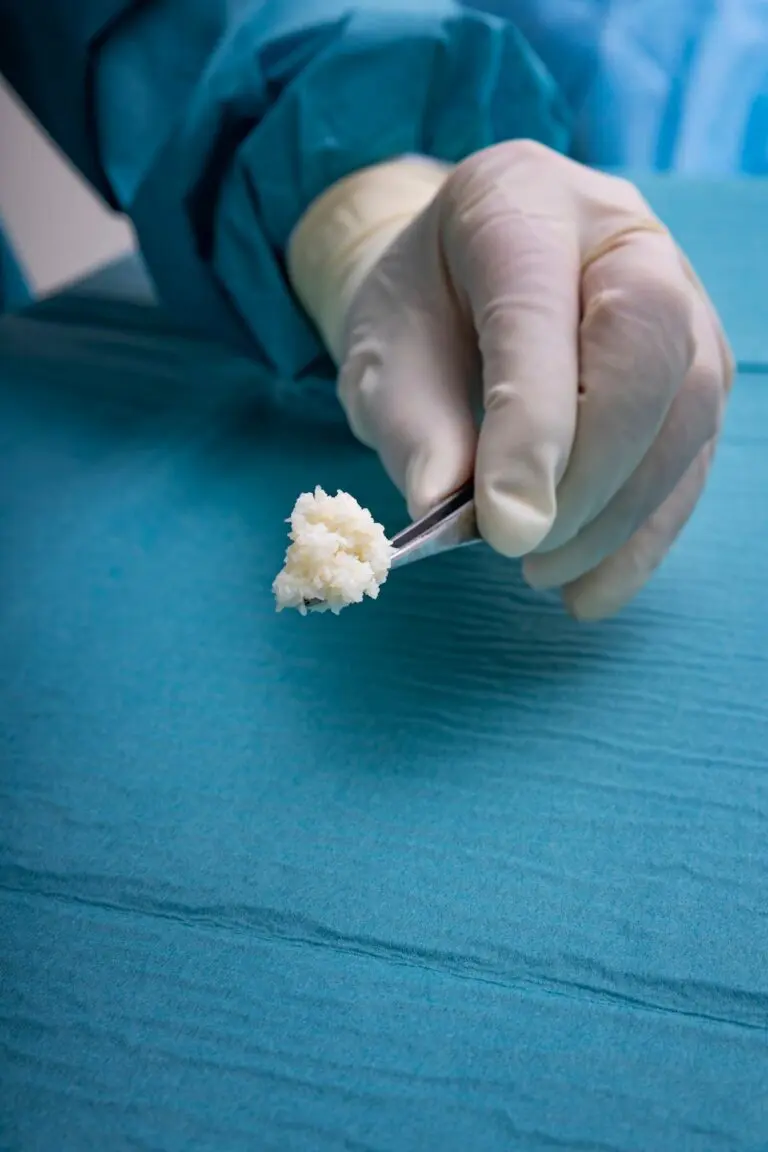
SurgiClose Micro is intact fish skin that has been fragmented. It offers more surface area than the non-fragmented version, and is designed to adhere to, fill deep wound spaces and irregular geometries.
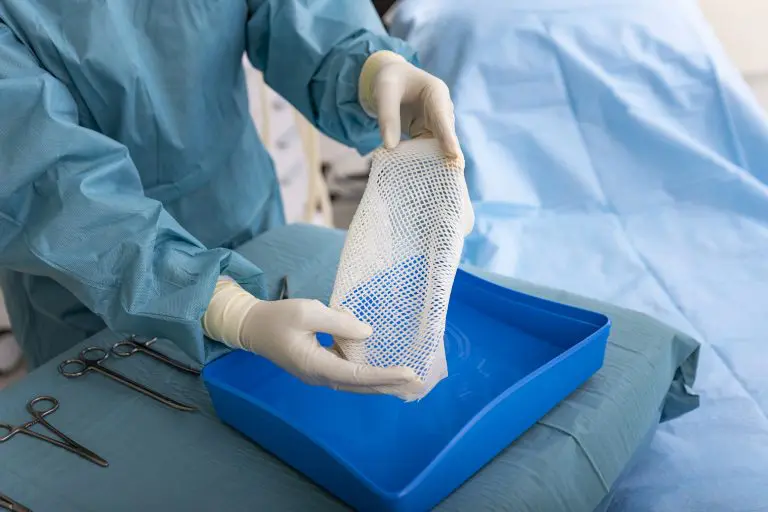
Meshed 2:1
2:1 pre-meshed intact fish skin graft is designed to expand and cover larger wounds. It provides a viable clinical and economic solution for large wounds.
Intended Use
Kerecis® SurgiClose® is indicated for the management of wounds including:
- Partial and full thickness wounds
- Pressure ulcers
- Chronic vascular ulcers
- Diabetic ulcers
- Trauma wounds (abrasions, lacerations, second-degree burns, skin tears)
- Surgical wounds (donor site/grafts, post-Mohs surgery, post-laser surgery, podiatric, wound dehiscence)
- Draining wounds
Instructions for Use – SurgiClose (USA)
Instructions for Use – SurgiClose Silicone (USA)

Need more information?
From the town of Ísafjörður in northwest Iceland, Kerecis develops, manufactures, and distributes patented fish-skin medical devices that support soft tissue regeneration in the body, with regulatory clearance in the United States, Europe, and beyond.
Important Information
Magnusson, S. et al. Regenerative and Antibacterial Properties of Acellular Fish Skin Grafts and Human Amnion/Chorion Membrane: Implications for Tissue Preservation in Combat Casualty Care. Mil. Med. 182, 383–388 (2017).
Baldursson, B. T. et al. Healing rate and autoimmune safety of full-thickness wounds treated with fish skin acellular dermal matrix versus porcine small-intestine submucosa: a non-inferiority study. Int. J. Low. Extrem. Wounds 14, (2015).
Magnusson, S. et al. Decellularized fish skin: characteristics that support tissue repair. Laeknabladid 101, 567–573 (2015)
Alam, K. & Jeffery, S. L. A. Acellular Fish Skin Grafts for Management of Split Thickness Donor Sites and Partial Thickness Burns: A Case Series. Mil Med. 184(Suppl 1):16-20 (2019).
Pujji, O. & Jeffery, S. L. A. Safe burn excision prior to military repatriation: an achievable goal? BMJ Military Health.164: 358-359 (2018).
Shupp, J. W. et al. Fish Skin Compared to Cadaver Skin as a Temporary Covering for Full Thickness Burns: An Early Feasibility Trial. Poster presented at: AMUS 2020 Annual Meeting (2020).
Badois, N. et al., Acellular fish skin matrix on thinskin graft donor sites: a preliminary study. J Wound Care 28. 624–628 (2019).
Kirsner, R. S. et al. Fish skin grafts compared to human amnion/chorion membrane allografts: A double-blind, prospective, randomized clinical trial of acute wound healing. Wound Repair Regen. 28, 75–80 (2020).
Lantis, J.C, 2nd, et al. Final efficacy and cost analysis of a fish skin graft vs standard of care in the management of chronic diabetic foot ulcers: a prospective, multicenter, randomized controlled clinical trial. Wounds. 35(4): 71-79 (2023).
Wallner, C. et al. A Comparison of Intact Piscine Skin, Split-thickness Skin Graft, and Lactic Acid Membrane in Treating Superficial and Deep Burn Wounds Following Enzymatic Debridement, J Burn Care Res. 42 (Suppl 1): 125-126 (2021).
Stone, R. 2nd, et al. Omega-3 Rich Fish Skin Grafts Reduce Donor Skin Requirements for Full Thickness Burns. J. Burn Care Res. 39, S234–S235 (2018).
Stone, R. 2nd, et al. Accelerated Wound Closure of Deep Partial Thickness Burns with Acellular Fish Skin Graft. Int J Mol Sci. 2021;22(4):1590 (2021).
Evangelatov, A., & Pankov, R. The evolution of three-dimensional cell cultures towards unimpeded regenerative medicine and tissue engineering. In Andrades, J. A. [Ed.] Regenerative medicine and tissue engineering. IntechOpen (2013).
Wang, Y. et al. Burn injury: challenges and advances in burn wound healing, infection, pain and scarring. Advanced drug delivery reviews, 123, 3-17 (2018).
Dardari D, Piaggesi A, Potier L, Sultan A, Diener H, Francois M, Dorweiler B, Bouillet B, M’Bemba J, Chaillous L, Clerici G, Kessler L, Wetzel-Roth W, Storck M, Davidsson OB, Baldursson B, Kjartansson H, Lantis JC, Charpentier G. Intact Fish Skin Graft to Treat Deep Diabetic Foot Ulcers. NEJM Evid. 2024 Oct 4, doi: 10.1056
*Image on left: Data on file. Image on right: Copyright Steve Gschmeissner/Science Photo Library.